Chiropractor Ypsilanti MI
Welcome to Hesselberg Chiropractic located in Ypsilanti. Chiropractic is one of the most amazing healthcare professions, but very few people understand what it's all about. This article is here to help you gain a basic understanding of how our Ypsilanti chiropractors can help you and your family.
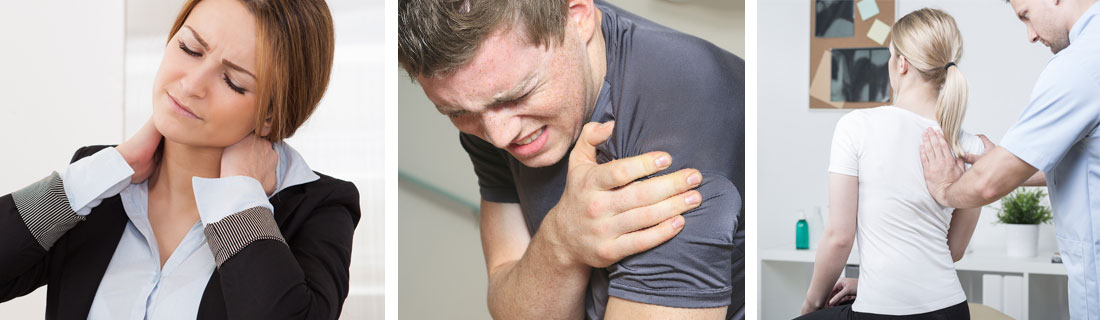
Chiropractic care is the practice of using spinal alignment to alleviate a wide variety of physical ailments, including muscle strain, neck pain, chronic back pain, and more. This is accomplished by adjusting the position of the spinal column to its proper shape, providing a non-invasive solution for pain relief.
We accept most insurances.
We're conveniently located on Packard Road across the street from the Washtenaw Golf Club.
Hesselberg Chiropractic
OFFICE HOURS
Monday
9:00am - 12:30pm
2:00pm - 6:00pm
Tuesday
9:00am - 12:30pm
2:00pm - 5:30pm
Wednesday
9:00am - 12:30pm
2:00pm - 6:00pm
Thursday
9:00am - 12:30pm
2:00pm - 5:30pm
Friday
12:00pm - 3:00pm
Saturday
9:00am - 12:00pm
Hesselberg Chiropractic
2900 Packard Street #2
Ypsilanti, MI 48197
(734) 677-0111
THE HISTORY OF CHIROPRACTIC CARE
The word “Chiropractic” is derived from the Greek words “cheir” (hand) and “praktos” (done) combined to mean “done by hand.” It was chosen by the developer of chiropractic care, Daniel David Palmer. In 1895, D.D. Palmer performed a chiropractic adjustment on a partially deaf janitor, Harvey Lillard, who later reported that his hearing had improved due to the change.
D.D. Palmer opened the first chiropractic school two years later, and in the century since, chiropractic professionals have used spinal adjustments to help people prevent and cope with back pain, carpal tunnel, muscle strain, headaches and migraines, and a variety of other physical ailments. Millions of people benefit from the work of Dr. Palmer today.
what kind of training does a chiropractor have?
Chiropractic doctors go through a minimum of four years of schooling at a chiropractic college, generally preceded by an undergraduate degree in the basic sciences or several years of experience in a prior relevant health care field.
Students of chiropractic care must spend a minimum of at least 4,200 hours with their teacher, and a minimum of 1,000 hours of fully supervised clinical training with an instructor as they learn the appropriate diagnosis and treatment techniques to help heal your body and restore it to its natural, fully functioning state.
Hesselberg Chiropractic Receives 2009, 2010 and 2011 Best of Ypsilanti Award






